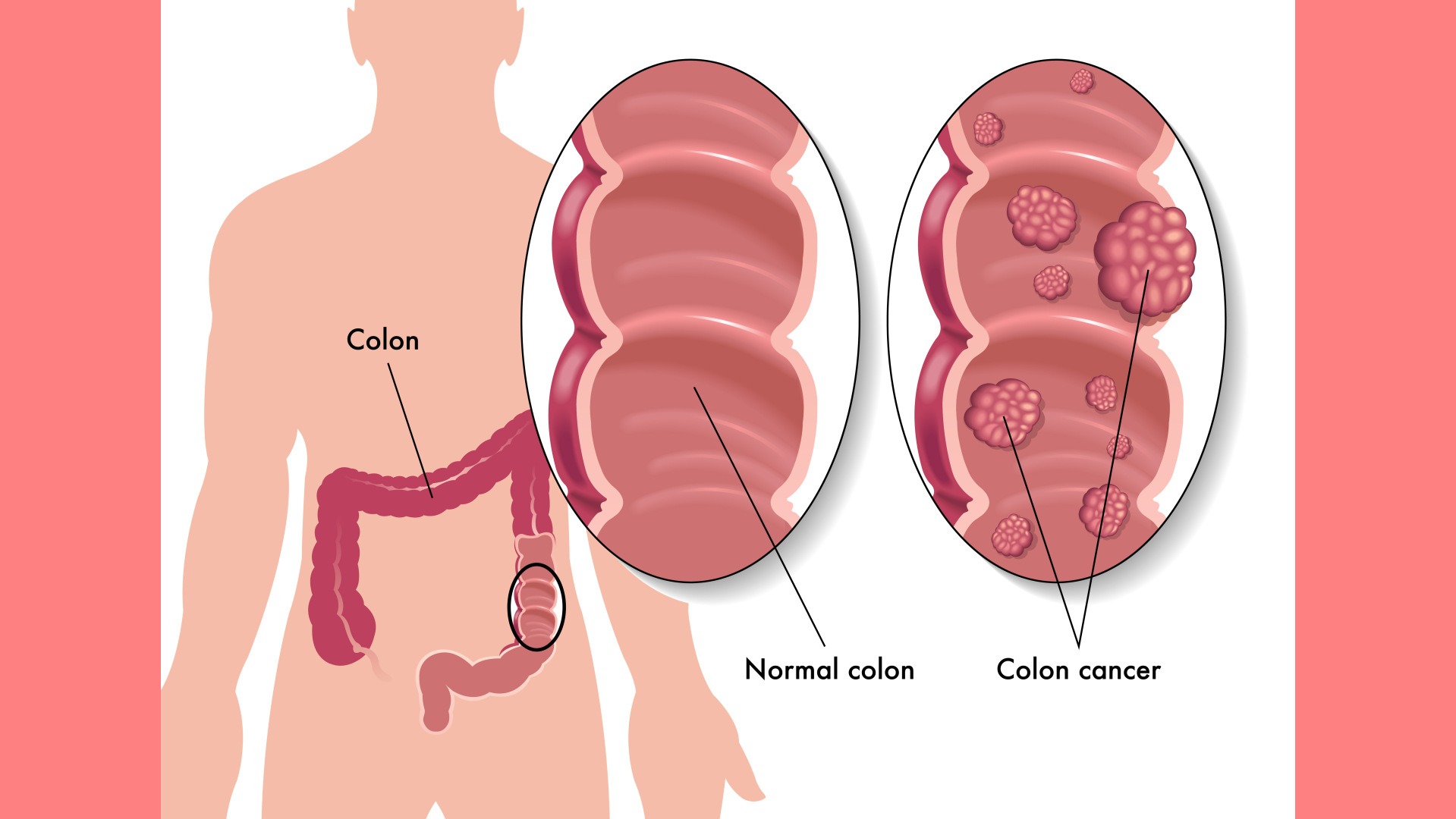
Colon cancer begins in your large intestine or the colon. The large intestine is a long tube that carries the digested food from your small intestine to your rectum. Your large intestine wall comprises layers of mucus membrane, muscle, and tissue. Colon cancer develops in the colon’s innermost lining, called the mucosa. Mucosa cells produce mucus and other fluids. Under certain conditions, these cells change and form colon polyps.
Colon cancer originates from colon polyps. These colon polyps can become cancerous. If undetected or untreated, the cancer makes its way through the muscle and the outer layer of your colon. Then, colon cancer can spread to other body parts via your lymph nodes and blood vessels.
One of the most distressing issues with colon cancer is the unbearable pain. Homeopathic remedies can help you with this pain without any side effects. Also, cancer detection can cause anxiety, depression, and fear. Homeopathy can help you deal with these emotions.
Role of homeopathy in colon cancer
There are different approaches used in homeopathy for treating colon cancer, depending on the type and severity of the colon cancer. The most common approach is prescribing a constitutional homeopathic remedy for colon cancer. These are prescribed on an individual constitutional basis and act as supportive and palliative solutions for colon cancer. The second approach for colon cancer is colon-specific medicines. These remedies target the cancer-affected colon to protect and manage it.
Top five homeopathic medicines for colon cancer
Aloe socotrina (Aloe.)
Common name: Socotrine aloes
Aloe socotrina is indicated when persistent diarrhea is the symptom in patients with colon cancer. There is an urgency to pass stool, more in the morning, after eating or drinking. Cutting pains in the rectum are preceded and accompanied by stools. The pain gets better after passing stools.
This remedy works well for those with a constant bearing down sensation in the rectum. Aloe. soc. works well in bloody stools with intense burning in the rectum and anus. A stool with jelly-like mucus passes involuntarily. This remedy works wonders in people with lumpy and watery stools with weakness, sweating, and fainting after passing stool.
Nitricum acidum (Nit-ac.)
Common name: Nitric acid
Nitric acid suits patients with colon cancer with intense pain in the rectum while passing stool. This is accompanied by tearing or cutting pain in the abdomen.
You may need to strain a lot to pass a dry, hard stool. The straining is so intense that the rectum feels torn, yet they pass very little stool. This abdominal pain continues for hours after stool. This remedy works for bright red bleeding from the rectum along with the stool.
Alumina (Alum.)
Common name: Pure clay
Alumina is indicated for colon cancer with constant constipation without any urge to defecate for several days. No passage of stools for several days due to slow and sluggish intestinal actions.
The stools are passed when a large quantity of fecal matter accumulates in the intestine. Excessive straining to pass stool, even if stools are soft, is the characteristic symptom of Alumina.
Phosphorus (Phos.)
Common name: Phosphorus
Phosphorus is given for colon cancer with bloody diarrhea and weakness. There is extreme exhaustion after passing stool.
Phosphorus is indicated for stools that are copious, gushing, and watery. There is painless rectal bleeding with the stools. The bleeding is often copious and bright red.
The stools are watery, yellowish, and offensive. There can be cramping pain in the rectum after passing stool.
Mercurius solubilis (Merc.)
Common name: Quicksilver
Merc. sol. works well in cases of colon cancer with blood in stools. There is a constant urge to evacuate the bowels and pass frequent loose stools. However, even after passing stool several times, there is no relief. It is indicated in cases of colon cancer with excessive burning and intense pain in the abdomen.
Causes for colon cancer
Like all kinds of cancers, colon cancer develops when colon cells grow and multiply uncontrollably. Healthy cells in your body are born, grow, divide, and die at a fixed pace. However, in colon cancer, cells of your colon lining keep growing and dividing and don’t die. In colon cancer, these cells may develop from colon polyps. Why some polyps develop into colon cancer is not clear yet. However, certain factors increase the risk of developing colon cancer. These risk factors include:
Race
African Americans have a higher risk of colon cancer than other races.
Smoking
Tobacco smoking, cigarettes, and chewing tobacco increase your risk for colon cancer.
Alcohol
Consuming excess alcohol can put you at a higher risk of developing colon cancer.
Obesity
Being overweight is known to increase the chances of colon cancer.
Diet
Consuming high-fat, high-calorie foods, red meat, and processed meat can increase your chances of colon cancer.
Inflammatory bowel disease
If you have inflammatory conditions like chronic ulcerative colitis and Crohn’s disease for years, it can put you at high risk of colon cancer.
Diabetes
If you have diabetes or have insulin resistance, it can elevate the risk of colon cancer.
Genetics
Colon cancer develops if you have inherent genetic diseases like Lynch syndrome and familial adenomatous polyposis.
Family history
If your close family members, like biological parents, siblings, and children, have colon cancer, you may have an increased risk of developing it.
Family history of polyp
If your close family member has a large and advanced polyp, you can be at higher risk for developing colon cancer.
Radiation therapy
Previous radiation therapies to treat abdominal cancers can also increase the chances of colon cancer.
Symptoms of colon cancer
Blood in stool
Blood in stool might be seen in two ways. You might notice blood in your toilet pot after you poop or on toilet paper after wiping or your stool may look dark or bright red.
Change in your bowel movements
You might experience constant changes in your bowel habits. It can be persistent constipation, diarrhea, or an ineffectual urge to defecate.
Abdominal pain
Unusual and frequent pain in your abdomen with no known cause could be a symptom of colon cancer. This kind of pain doesn’t go away or might increase in intensity.
Bloating
Persistent bloating that lasts for weeks or worsens can be an alarming symptom. Bloating in colon cancer is accompanied by vomiting or blood in stools.
Unexplained weight loss
Sudden, unusual, and noticeable drops in your body weight can be a symptom of colon cancer.
Vomiting
Colon cancer may present with periodic vomiting without any apparent reason.
Fatigue and breathlessness
Colon cancer can lead to anemia. Due to anemia, you might feel tired and breathless.
Treatment for colon cancer
Many cases of colon cancer are treated with surgery. The different surgeries and procedures include:
Polypectomy
Cancerous polyps are removed in polypectomy.
Partial colectomy
In this resection surgery, a section of your colon that contains a tumor is removed. After this surgery, your healthy colon sections are reconnected.
Surgical resection with colostomy
This is similar to colectomy, where a section of your colon containing a tumor is removed. However, the colon sections are not reconnected and an opening is made in your abdominal wall. A colostomy bag that helps collect stools is attached to this opening.
Radiofrequency ablation
Heat is used to destroy colon cancer cells in radiofrequency ablation.
Colon surgery is often given with adjuvant therapy before or after surgery. These treatments may include:
Chemotherapy
Chemotherapy drugs are used to shrink your tumors and relieve colon cancer symptoms.
Targeted therapy
The genes, proteins, and tissues that help colon cancer cells grow and multiply are eliminated in targeted therapy.
Diet and lifestyle management for colon cancer
Quit smoking
Avoid or quit nicotine smoking to prevent your colon cancer from worsening.
Decrease alcohol intake
Drink alcoholic beverages in moderation. If you are a man, limit alcohol to two servings a day. If you are a woman, limit alcohol to one serving a day.
Healthy diet
Add seasonal fruit and vegetables to your diet and reduce high-fat and high-calorie foods, processed foods, and red meat. Drinking coffee can lower your risk of colon cancer.
Colon cancer screening
If you have a family history of colon cancer, colon polyps, or chronic irritable bowel disease, get annual screening before the age of 45.
Conclusion
Genetic mutations cause abnormal cell growth in colon cancer. Timely screening can help in early detection and treatment before it spreads.
Homeopathy can be one of the complementary modes of management for colon cancer. Integrating homeopathy with conventional treatments will help you have a better quality of life.
References
- Augustus GJ, Ellis NA. Colorectal cancer disparity in African Americans. Am J Pathol [Internet]. 2018 [cited 2024 Jan 21];188(2):291–303. Available from: http://dx.doi.org/10.1016/j.ajpath.2017.07.023
- Gram IT, Park S-Y, Wilkens LR, Haiman CA, Le Marchand L. Smoking-related risks of colorectal cancer by anatomical subsite and sex. Am J Epidemiol [Internet]. 2020 [cited 2024 Jan 21];189(6):543–53. Available from: http://dx.doi.org/10.1093/aje/kwaa005
- Park S-Y, Wilkens LR, Setiawan VW, Monroe KR, Haiman CA, Le Marchand L. Alcohol intake and colorectal cancer risk in the multiethnic cohort study. Am J Epidemiol [Internet]. 2019 [cited 2024 Jan 21];188(1):67–76. Available from: http://dx.doi.org/10.1093/aje/kwy208
- Frezza EE. Influence of obesity on the risk of developing colon cancer. Gut [Internet]. 2006 [cited 2024 Jan 21];55(2):285–91. Available from: http://dx.doi.org/10.1136/gut.2005.073163
- Gillen CD, Walmsley RS, Prior P, Andrews HA, Allan RN. Ulcerative colitis and Crohn’s disease: a comparison of the colorectal cancer risk in extensive colitis. Gut [Internet]. 1994 [cited 2024 Jan 21];35(11):1590–2. Available from: http://dx.doi.org/10.1136/gut.35.11.1590
- Yu G-H, Li S-F, Wei R, Jiang Z. Diabetes and colorectal cancer risk: Clinical and therapeutic implications. J Diabetes Res [Internet]. 2022 [cited 2024 Jan 21];2022:1–16. Available from: http://dx.doi.org/10.1155/2022/1747326
- Jasperson KW, Tuohy TM, Neklason DW, Burt RW. Hereditary and familial colon cancer. Gastroenterology [Internet]. 2010 [cited 2024 Jan 21];138(6):2044–58. Available from: http://dx.doi.org/10.1053/j.gastro.2010.01.054
- Henrikson NB, Webber EM, Goddard KA, Scrol A, Piper M, Williams MS, et al. Family history and the natural history of colorectal cancer: systematic review. Genet Med [Internet]. 2015 [cited 2024 Jan 21];17(9):702–12. Available from: http://dx.doi.org/10.1038/gim.2014.188
- Song M, Emilsson L, Roelstraete B, Ludvigsson JF. Risk of colorectal cancer in first degree relatives of patients with colorectal polyps: nationwide case-control study in Sweden. BMJ [Internet]. 2021 [cited 2024 Jan 21];373:n877. Available from: http://dx.doi.org/10.1136/bmj.n877
- Sasaki K, Ishihara S, Hata K, Kiyomatsu T, Nozawa H, Kawai K, et al. Radiation-associated colon cancer: A case report. Mol Clin Oncol [Internet]. 2017 [cited 2024 Jan 21];6(6):817–20. Available from: http://dx.doi.org/10.3892/mco.2017.1252
- Zauber AG, Winawer SJ, O’Brien MJ, Lansdorp-Vogelaar I, van Ballegooijen M, Hankey BF, et al. Colonoscopic polypectomy and long-term prevention of colorectal-cancer deaths. N Engl J Med [Internet]. 2012 [cited 2024 Jan 21];366(8):687–96. Available from: http://dx.doi.org/10.1056/nejmoa1100370
- Tanabe KK, Kulu Y. Radiofrequency ablation for colon and rectal carcinoma liver metastases: What’s missing? Gastrointestinal Cancer Research?: GCR. 2007;1(4 Suppl 2):S42. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2666846/
- Gonzalez-Angulo AM, Fuloria J. The role of chemotherapy in colon cancer. The Ochsner Journal. Available from: 2002;4(3):163.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3399277/
- Ohishi T, Kaneko MK, Yoshida Y, Takashima A, Kato Y, Kawada M. Current targeted therapy for metastatic colorectal cancer. Int J Mol Sci [Internet]. 2023 [cited 2024 Jan 21];24(2):1702. Available from: http://dx.doi.org/10.3390/ijms24021702
- Gram IT, Park S-Y, Wilkens LR, Haiman CA, Le Marchand L. Smoking-related risks of colorectal cancer by anatomical subsite and sex. Am J Epidemiol [Internet]. 2020 [cited 2024 Jan 21];189(6):543–53. Available from: http://dx.doi.org/10.1093/aje/kwaa005
- Park S-Y, Wilkens LR, Setiawan VW, Monroe KR, Haiman CA, Le Marchand L. Alcohol intake and colorectal cancer risk in the multiethnic cohort study. Am J Epidemiol [Internet]. 2019 [cited 2024 Jan 21];188(1):67–76. Available from: http://dx.doi.org/10.1093/aje/kwy208
- Jin H, Zhang C. High fat high calories diet (HFD) increase gut susceptibility to carcinogens by altering the gut microbial community. J Cancer [Internet]. 2020 [cited 2024 Jan 21];11(14):4091–8. Available from: http://dx.doi.org/10.7150/jca.43561
- Chan DSM, Lau R, Aune D, Vieira R, Greenwood DC, Kampman E, et al. Red and processed meat and colorectal cancer incidence: Meta-analysis of prospective studies. PLoS One [Internet]. 2011 [cited 2024 Jan 21];6(6):e20456. Available from: https://pubmed.ncbi.nlm.nih.gov/21674008/
- Schmit SL, Rennert HS, Rennert G, Gruber SB. Coffee consumption and the risk of Colorectal Cancer. Cancer Epidemiol Biomarkers Prev [Internet]. 2016 [cited 2024 Jan 21];25(4):634–9. Available from: http://dx.doi.org/10.1158/1055-9965.epi-15-0924