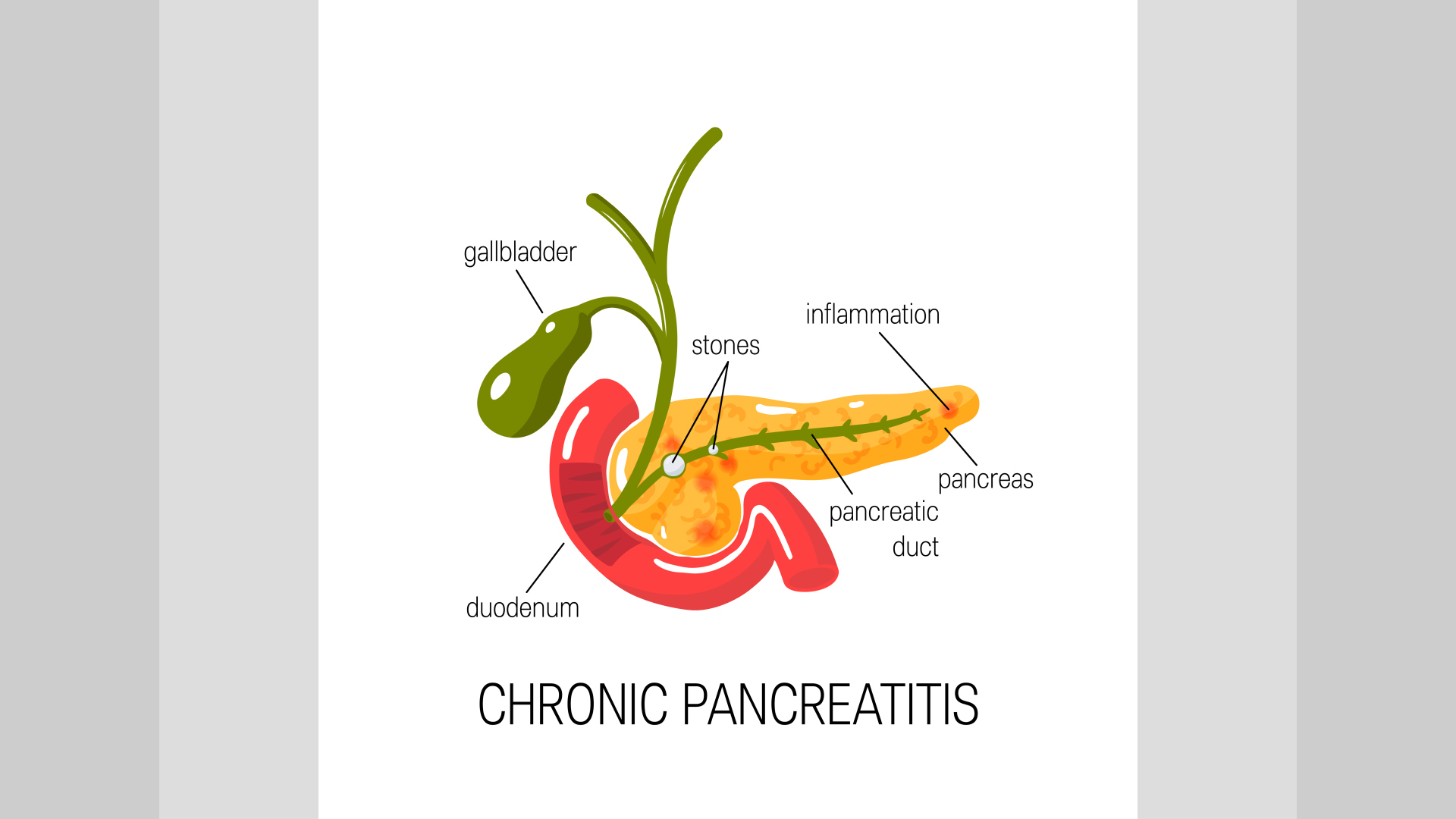
Pancreatitis is a condition characterized by inflammation of the pancreas. The pancreas is a long, flat gland behind your stomach in the upper abdomen. It performs both exocrine and endocrine functions in your body. The enzymes, pancreatic protease, lipase, and serum amylase produced by your pancreas, help in digestion. Pancreatic hormones (insulin and glucagon) regulate your blood sugar levels.
Pancreatitis can be of two types: acute or chronic. In acute pancreatitis, there is a sudden and short-term inflammation. However, the pancreas has long-lasting inflammation lasting for months or years in chronic pancreatitis.
The most common causes of pancreatitis include excess alcohol consumption and gallstone formation. You may also develop chronic pancreatitis if you smoke, have high levels of calcium or triglycerides, injury, infection, narrow or blocked pancreatic ducts, cystic fibrosis, and certain medications.
Homeopathy aims to treat chronic pancreatitis by addressing its underlying cause. Homeopathic remedies are selected based on the cause, sensations, and modalities of pancreatitis. However, consulting a qualified homeopathic doctor is essential to get individualized medicine.
Role of homeopathy in chronic pancreatitis
Homeopathy is a supportive treatment in the case of chronic pancreatitis. In chronic pancreatitis, the inflammatory response damages your pancreatic cells. Homeopathy acts by correcting the root cause of your chronic pancreatitis. This relieves your symptoms of chronic pancreatitis and may help improve your pancreatic function.
Top five homeopathic medicines for chronic pancreatitis
Arsenic album (Ars. alb.)
Common name: Arsenious acid
Ars. alb. is an indicated medicine for chronic pancreatitis with nausea, vomiting, and diarrhea. Vomiting is induced by eating or drinking any food. This vomit tastes bitter and is greenish yellow in color. There is constant nausea along with vomiting.
Ars. alb. is suited for chronic pancreatitis with profuse, watery stools mixed with mucus and undigested food. The diarrhea worsens after eating and at midnight. There is a loss of appetite and marked weakness due to profuse diarrhea. Abdominal pains of cutting, tearing, or burning in nature, along with the above symptoms, are characteristics of this remedy.
Belladonna (Bell.)
Common name: Deadly Nightshade
Belladonna is indicated for abdominal pain due to chronic pancreatitis. The pain is often gripping, pinching, cutting, or clutching. Abdominal pain often worsens from the slightest movement. Belladonna is well-indicated for severe abdominal pain that is relieved by pressing the abdomen. The pain comes on suddenly, lasts for a shorter duration, and disappears suddenly.
Heat and sensitivity in the abdomen are other associated symptoms. The sensitivity is so high that the slightest touch worsens the pain.
Colocynthis (Coloc.)
Common name: Bitter cucumber
Colocynthis is effective for abdominal pain due to chronic pancreatitis. The pain begins in the upper part of the abdomen and is colicky or cutting in nature. The abdomen has marked sensitivity where even the slightest touch causes pain.
Colocynthis works well in chronic pancreatitis pain that worsens after drinking or eating a small amount of food. This pain is relieved by bending forward and applying hard pressure on the abdomen. Abdominal pain followed by a watery stool is the characteristic symptom of Colocynthis.
Iris versicolor (Iris)
Common name: Blue flag
Iris versicolor is considered in cases of chronic pancreatitis with burning distress in the pancreatic region. The patient feels severe burning, and even drinking cold water does not give any relief.
Iris versicolor is indicated in chronic pancreatitis with greasy or fatty stool. There is marked abdominal colic associated with watery diarrhea and sweetish vomiting. This pain is relieved by bending forward and by passing flatus.
Leptandra Virginia (Lept.)
Common name: Culver’s root
Leptandra is indicated for chronic pancreatitis with jaundice. There is nausea and bilious vomiting due to jaundice. There is a loss of appetite and excessive fatigue. Leptandra is prescribed for diarrhea that worsens in the morning.
Causes for chronic pancreatitis
Gallstone
Bile from your gallbladder is emptied into your intestine through your common bile duct. When a gallstone enters your common bile duct, it may get stuck at that junction. This temporarily blocks the drainage of pancreatic juice and traps the enzymes inside your pancreas. As pressure increases due to obstruction, it activates the enzymes inside your pancreas. These enzymes begin digesting your pancreas itself, causing chronic pancreatitis.
Alcohol
Alcohol consumption can cause pancreatitis. The toxic byproducts of alcohol and its effects on your blood cause pancreatic inflammation. This activates the digestive enzymes within your pancreas, leading to chronic pancreatitis.
Infections
Viral infections, like mumps or hepatitis, can trigger inflammatory responses in your pancreas, leading to chronic pancreatitis.
Autoimmune disease
Your immune system can mistakenly attack your pancreatic cells, causing inflammation and chronic pancreatitis.
Genetic mutations
Specific genetic mutations in the CTSB gene running in your family can put you at high risk for developing chronic pancreatitis.
Cystic fibrosis
In cystic fibrosis, sticky and thick mucus in your pancreatic ducts obstructs the ducts and triggers chronic pancreatitis.
High triglyceride levels
Elevated triglyceride levels in your blood can cause fat to accumulate in your pancreas. This contributes to inflammation, causing chronic pancreatitis.
High blood calcium levels
Excess calcium in your blood can lead to pancreatic inflammation and chronic pancreatitis.
Ischemia
Reduced blood flow to your pancreas due to vascular issues can result in ischemic chronic pancreatitis.
Cancer
Tumors in or near your pancreas can obstruct bile ducts and cause inflammation, leading to chronic pancreatitis.
Symptoms of chronic pancreatitis
The prominent symptom of chronic pancreatitis is abdominal pain. This pain can be moderate to severe in intensity and often radiates to your back. You may feel the tenderness in your abdomen. In chronic pancreatitis, the pain doesn’t persist; it comes and goes but doesn’t go away completely. You may notice it more when you eat, lie flat, cough, or exercise. Your pain improves when you sit upright, lean forward, and eat less.
Other symptoms of chronic pancreatitis include:
- Nausea and vomiting
- Indigestion
- Pain after eating
- Increased heart rate
- Shallow breathing
- Fever
- Loss of appetite
- Unexplained weight loss
- Fatty stools
- Lightheadedness
Management for chronic pancreatitis
IV fluids
An acute episode of chronic pancreatitis can dehydrate you. Hydration is essential for healing chronic pancreatitis. IV fluids are used to manage pancreatitis.
Tube feeding
Decreased appetite, nausea, vomiting, and diarrhea can affect your nutrition in chronic pancreatitis. If you cannot eat food by mouth, doctors administer food through a tube placed via your nose or stomach to provide you with enough nutrition.
Nutritional supplements
Healthcare professionals may recommend nutritional supplements, such as pancreatic enzyme supplements, to aid digestion.
Pain management
Analgesics are given orally or through an IV directly into your bloodstream. However, long-term pain relief can be complex. You will be referred to a chronic pain specialist to manage long-term pain.
Endoscopy
Removing scar tissue or pancreatic stones by endoscopy can relieve your symptoms of chronic pancreatitis.
Gallstone removal
Gallstone removal or gallbladder removal surgery is recommended to prevent complications and chronic pancreatitis recurrence.
Diet and lifestyle changes for chronic pancreatitis
Low-fat diet
Reduce your intake of high-fat foods, as fats can stimulate the pancreas and worsen symptoms. Switch to a low-fat diet to prevent recurring pain attacks in chronic pancreatitis.
Small, frequent meals
Eat smaller, more frequent meals instead of large portions, throughout the day to decrease the workload on your pancreas.
Hydration
Drink sufficient quantities of water, as dehydration can worsen chronic pancreatitis.
Avoid trigger foods
Identify and avoid specific foods that may trigger or worsen inflammation. Common triggers include spicy foods and high-fat or fried foods.
Avoid alcohol
Avoid alcohol entirely if you have chronic pancreatitis.
Weight management
Maintain an optimum body weight with the help of a balanced diet and regular exercise. Obesity can cause or worsen chronic pancreatitis.
Quit smoking
Avoid smoking as it puts you at a high risk for chronic pancreatitis and can worsen the condition.
Conclusion
Chronic pancreatitis can disrupt your routine activities. Its treatment involves a multifaceted approach combining medical treatment along with dietary and lifestyle modifications.
Homeopathy is the supportive mode of treatment for chronic pancreatitis. Constitutional homeopathic medicines for chronic pancreatitis can relieve symptoms. This holistic approach can manage this condition and help you live a better life.
References
- Sohanraj Jain, Bipin & Nayak, Akshata. (2022). Homoeopathic management of chronic replapsing pancreatitis in a paediatric patient: A case report. Journal of Integrated Standardized Homoeopathy. 4. 133-141. 10. 25259/JISH_17_2021. Researchgate.net. [cited 2024 Jan 17]. Available from: https://www.researchgate.net/publication/357778764_Homoeopathic_management_of_chronic_replapsing_pancreatitis_in_a_paediatric_patient_A_case_rep
- Nanabhai, A. S., Vakil, Y. E., & Vakil, A. E. (1989). A study of Iris versicolor 3c. The British Homoeopathic Journal, 78(01), 15–18. https://doi.org/10.1016/s0007-0785(89)80125-5
- Yan M-X, Li Y-Q. Gall stones and chronic pancreatitis: the black box in between. Postgrad Med J [Internet]. 2006 [cited 2024 Jan 17];82(966):254–8. Available from: http://dx.doi.org/10.1136/pgmj.2005.037192
- Klochkov A, Kudaravalli P, Lim Y, Sun Y. Alcoholic Pancreatitis. StatPearls Publishing; 2023.https://www.ncbi.nlm.nih.gov/books/NBK537191/
- Sarshari B, Zareh-Khoshchehreh R, Keshavarz M, Manshadi SAD, SeyedAlinaghi S, Aghdaei HA, et al. The possible role of viral infections in acute pancreatitis: a review of literature. Gastroenterology and Hepatology From Bed to Bench [Internet]. 2023 [cited 2024 Jan 17];16(3):270. Available from: http://dx.doi.org/10.22037/ghfbb.v16i2.2582
- Fan B-G, Andrén-Sandberg Å. Autoimmune pancreatitis. North American Journal of Medical Sciences. 2009;1(4):148.Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3364658/
- Ravi Kanth VV. Genetics of acute and chronic pancreatitis: An update. World J Gastrointest Pathophysiol [Internet]. 2014 [cited 2024 Jan 17];5(4):427. Available from: http://dx.doi.org/10.4291/wjgp.v5.i4.427
- Witt H. Chronic pancreatitis and cystic fibrosis. Gut [Internet]. 2003 [cited 2024 Jan 17];52(90002):31ii–41. Available from: http://dx.doi.org/10.1136/gut.52.suppl_2.ii31
- de Pretis N, Amodio A, Frulloni L. Hypertriglyceridemic pancreatitis: Epidemiology, pathophysiology and clinical management. United European Gastroenterol J [Internet]. 2018 [cited 2024 Jan 17];6(5):649–55. Available from: http://dx.doi.org/10.1177/2050640618755002
- Tiwari AK, Kumar V, Yadav DP, Shukla SK, Das D, Singh G, et al. Hypercalcemia – An enigmatic cause of acute pancreatitis. Journal of Clinical and Translational Research. 2022;8(3):176.Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9260341/
- Yaowmaneerat T, Sirinawasatien A. Update on the strategy for intravenous fluid treatment in acute pancreatitis. World J Gastrointest Pharmacol Ther [Internet]. 2023 [cited 2024 Jan 17];14(3):22–32. Available from: http://dx.doi.org/10.4292/wjgpt.v14.i3.22
- Rasmussen HH. Nutrition in chronic pancreatitis. World J Gastroenterol [Internet]. 2013 [cited 2024 Jan 17];19(42):7267. Available from: http://dx.doi.org/10.3748/wjg.v19.i42.7267
- Kocher HM, Kadaba R. Chronic pancreatitis: dietary supplements. BMJ Clinical Evidence. 2015;2015.Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4548200/
- Gachago C, Draganov PV. Pain management in chronic pancreatitis. World J Gastroenterol [Internet]. 2008 [cited 2024 Jan 17];14(20):3137. Available from: http://dx.doi.org/10.3748/wjg.14.3137
- Tan DMY, Sherman S. Endoscopic therapy in chronic pancreatitis. Korean J Intern Med [Internet]. 2011 [cited 2024 Jan 17];26(4):384. Available from: http://dx.doi.org/10.3904/kjim.2011.26.4.384
- Hines JH, Pillai S. Gallstone pancreatitis post laparoscopic cholecystectomy: A case report. Cureus [Internet]. 2023 [cited 2024 Jan 17];15(5). Available from: http://dx.doi.org/10.7759/cureus.39704
- Ikeura T, Takaoka M, Uchida K, Miyoshi H, Okazaki K. Beneficial effect of low-fat elemental diet therapy on pain in chronic pancreatitis. Int J Chronic Dis [Internet]. 2014 [cited 2024 Jan 17];2014:1–5. Available from: http://dx.doi.org/10.1155/2014/862091
- W?ochal M, Swora-Cwynar E, Karczewski J, Grzymis?awski M. Assessment of nutritional knowledge of patients with pancreatitis. Prz Gastroenterol [Internet]. 2015 [cited 2024 Jan 17];4(4):229–33. Available from: http://dx.doi.org/10.5114/pg.2015.52402
- Sissingh NJ, Nagelhout A, Besselink MG, Boermeester MA, Bouwense SAW, Bruno MJ, et al. Structured alcohol cessation support program versus current practice in acute alcoholic pancreatitis (PANDA): Study protocol for a multicentre cluster randomised controlled trial. Pancreatology [Internet]. 2023;23(8):942–8. Available from: https://www.sciencedirect.com/science/article/pii/S1424390323018276
- Khatua B, El-Kurdi B, Singh VP. Obesity and pancreatitis. Curr Opin Gastroenterol [Internet]. 2017 [cited 2024 Jan 17];33(5):374–82. Available from: http://dx.doi.org/10.1097/mog.0000000000000386