Cholecystitis is inflammation of the gall bladder.
Causes and pathology of Cholecystitis
Cholecystitis is often caused by cholelithiasis (the presence of choleliths, or gallstones, in the gallbladder), with choleliths most commonly blocking the cystic duct directly. This leads to inspissation of bile, bile stasis, and secondary infection by gut organisms, predominantly E coli and Bacteroides species.
The gallbladder’s wall becomes inflamed. Extreme cases may result in necrosis and rupture. Inflammation often spreads to its outer covering, thus irritating surrounding structures such as the diaphragm and bowel.
Less commonly, in debilitated and trauma patients, the gallbladder may become inflamed and infected in the absence of cholelithiasis, and is known as acute acalculous cholecystitis.
Stones in the gallbladder may not cause obstruction and the accompanying acute attack. The patient might develop a chronic, low-level inflammation which leads to a chronic cholecystitis, where the gallbladder is fibrotic and calcified.
Symptoms of Cholecystitis
Cholecystitis usually presents as a pain in the right upper quadrant. This is usually a constant, severe pain. The pain may be felt to ‘refer’ to the right flank or right scapular region at first.
This is usually accompanied by a low grade fever, vomiting and nausea.
More severe symptoms such as high fever, shock and jaundice indicate the development of complications such as abscess formation, perforation or ascending cholangitis. Another complication, gallstone ileus, occurs if the gallbladder perforates and forms a fistula with the nearby small bowel, leading to symptoms of intestinal obstruction.
Chronic cholecystitis manifests with non-specific symptoms such as nausea, vague abdominal pain, belching, diarrhea
Diagnosis for Cholecystitis
Cholecystitis is usually diagnosed by a history of the above symptoms, as well examination findings:
- fever (usually low grade in uncomplicated cases)
- tender right upper quadrant +/- Murphy’s sign
Subsequent laboratory and imaging tests are used to confirm the diagnosis and exclude other possible causes.
Differential diagnosis
Acute cholecystitis
- This should be suspected whenever there is acute right upper quadrant or epigastric pain.
- Other possible causes include:
- Perforated peptic ulcer
- Acute peptic ulcer exacerbation
- Amoebic liver abscess
- Acute amoebic liver colitis
- Acute pancreatitis
- Acute intestinal obstruction
- Renal colic
- Acute retrocolic appendicitis
- Other possible causes include:
Chronic cholecystitis
- The symptoms of chronic cholecystitis are non-specific, thus chronic cholecystitis may be mistaken for other common disorders:
- Peptic ulcer
- Hiatus hernia
- Colitis
- Functional bowel syndrome
quick differential
- biliary colic – cystic duct blocked. sharp and constant pain without fever. no murphy’s. LFT wnl. u/s
- cholecystitis – cystic duct blocked with infection. colicky brief pain at first, then constant pain in RUQ with fever caused by e coli, klebsiella, pseudomonas, b fragilis, enterococcus. murphy’s sign. increased AST, ALT, AP, WBC. u/s
- choledocholithiasis – common bile duct blocked. colicky pain. jaundice. increased bilirubin. cholangiogram.
- cholangitis – infection of entire biliary tract. charcot triad. jaundice and fever. increased AST, ALT, AP, bilirubin. cholangiogram.
Investigations for Cholecystitis
Blood
Laboratory values may be notable for an elevated alkaline phosphatase, possibly an elevated bilirubin (although this may indicate choledocholithiasis), and possibly an elevation of the WBC count. CRP (C-reactive protein) is often elevated. The degree of elevation of these laboratory values may depend on the degree of inflammation of the gallbladder. Patients with acute cholecystitis are much more likely to manifest abnormal laboratory values, while in chronic cholecystitis the laboratory values are frequently normal.
Radiology
Sonography is a sensitive and specific modality for diagnosis of acute cholecystitis; adjusted sensitivity and specificity for diagnosis of acute cholecystitis are 88% and 80%, respectively. The 2 major diagnostic criteria are cholelithiasis and sonographic Murphy’s sign. Minor criteria include gallbladder wall thickening greater than 3mm, pericholecystic fluid, and gallbladder dilatation.
The reported sensitivity and specificity of CT scan findings are in the range of 90-95%. CT is more sensitive than ultrasonography in the depiction of pericholecystic inflammatory response and in localizing pericholecystic abscesses, pericholecystic gas, and calculi outside the lumen of the gallbladder. CT cannot see noncalcified gallbladder calculi, and cannot assess for a Murphy’s sign.
Hepatobiliary scintigraphy with technetium-99m DISIDA (bilirubin) analog is also sensitive and accurate for diagnosis of chronic and acute cholecystitis. It can also assess the ability of the gall bladder to expel bile (gall bladder ejection fraction), and low gall bladder ejection fraction has been linked to chronic cholecystitis. However, since most patients with right upper quadrant pain do not have cholecystitis, primary evaluation is usually accomplished with a modality that can diagnose other causes, as well.
Therapy
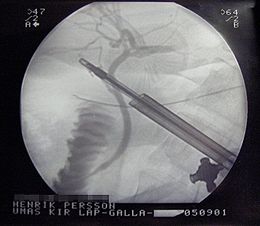
X-Ray during laparoscopic cholecystectomy
For most patients, in most centres, the definitive treatment is surgical removal of the gallbladder. Supportive measures are instituted in the meantime and to prepare the patient for surgery. These measures include fluid resuscitation and antibiotics. Antibiotic regimens usually consist of a broad spectrum antibiotic such as piperacillin-tazobactam (Zosyn), ampicillin-sulbactam (Unasyn), ticarcillin-clavulanate (Timentin), or a cephalosporin (e.g.ceftriaxone) and an antibacterial with good coverage against anaerobic bacteria, such as metronidazole. For penicillin allergic patients aztreonam and clindamycin may be used.
Gallbladder removal, cholecystectomy, can be accomplished via open surgery or a laparoscopic procedure. Laparoscopic procedures can have less morbidity and a shorter recovery stay. Open procedures are usually done if complications have developed or the patient has had prior surgery to the area, making laparoscopic surgery technically difficult. A laparoscopic procedure may also be ‘converted’ to an open procedure during the operation if the surgeon feels that further attempts at laparoscopic removal might harm the patient. Open procedure may also be done if the surgeon does not know how to perform a laparoscopic cholecystectomy.
In cases of severe inflammation, shock, or if the patient has higher risk for general anesthesia (required for cholecystectomy), the managing physician may elect to have an interventional radiologist insert a percutaneous drainage catheter into the gallbladder (‘percutaneous cholecystostomy tube’) and treat the patient with antibiotics until the acute inflammation resolves. The patient may later warrant cholecystectomy if their condition improves.
Complications of cholecystitis
- Perforation or rupture
- Ascending cholangitis
Complications of cholecystectomy
- bile leak (“biloma”)
- bile duct injury (about 5-7 out of 1000 operations. Open and laparoscopic surgeries have essentially equal rate of injuries, but the recent trend is towards fewer injuries with laparoscopy. It may be that the open cases often result because the gallbladder is too difficult or risky to remove with laparoscopy)
- abscess
- wound infection
- bleeding (liver surface and cystic artery are most common sites)
- hernia
- organ injury (intestine and liver are at highest risk, especially if the gallbladder has become adherent/scarred to other organs due to inflammation (e.g. transverse colon)
- deep vein thrombosis/pulmonary embolism (unusual- risk can be decreased through use of sequential compression devices on legs during surgery)
Gall bladder perforation
Gall bladder perforation (GBP) is a rare but life-threatening complication of acute cholecystitis. The early diagnosis and treatment of GBP are crucial to decrease patient morbidity and mortality.
Approaches to this complication will vary based on the condition of an individual patient, the evaluation of the treating surgeon or physician, and the facilities’ capability. Perforation can happen at the neck from pressure necrosis due to the impacted calculus, or at the fundus. It can result in a local abscess, or perforation into the general peritoneal cavity. If the bile is infected, diffuse peritonitis may occur readily and rapidly and may result in death.
A retrospective study looked at 332 patients who received medical and/or surgical treatment with the diagnosis of acute cholecystitis. Patients were treated with analgesics and antibiotics within the first 36 hours after admission (with a mean of 9 hours), and proceeded to surgery for a cholecystectomy. Two patients died and 6 patients had further complications. The morbidity and mortality rates were 37.5% and 12.5%, respectively in the present study. The authors of this study suggests that early diagnosis and emergency surgical treatment of gallbladder perforation are of crucial importance.[1]
Homeopathy Treatment for Cholecystitis
Keywords: homeopathy, homeopathic, treatment, cure, remedy, remedies, medicine
Homeopathy treats the person as a whole. It means that homeopathic treatment focuses on the patient as a person, as well as his pathological condition. The homeopathic medicines are selected after a full individualizing examination and case-analysis, which includes the medical history of the patient, physical and mental constitution, family history, presenting symptoms, underlying pathology, possible causative factors etc. A miasmatic tendency (predisposition/susceptibility) is also often taken into account for the treatment of chronic conditions. A homeopathy doctor tries to treat more than just the presenting symptoms. The focus is usually on what caused the disease condition? Why ‘this patient’ is sick ‘this way’. The disease diagnosis is important but in homeopathy, the cause of disease is not just probed to the level of bacteria and viruses. Other factors like mental, emotional and physical stress that could predispose a person to illness are also looked for. No a days, even modern medicine also considers a large number of diseases as psychosomatic. The correct homeopathy remedy tries to correct this disease predisposition. The focus is not on curing the disease but to cure the person who is sick, to restore the health. If a disease pathology is not very advanced, homeopathy remedies do give a hope for cure but even in incurable cases, the quality of life can be greatly improved with homeopathic medicines.
The homeopathic remedies (medicines) given below indicate the therapeutic affinity but this is not a complete and definite guide to the homeopathy treatment of this condition. The symptoms listed against each homeopathic remedy may not be directly related to this disease because in homeopathy general symptoms and constitutional indications are also taken into account for selecting a remedy. To study any of the following remedies in more detail, please visit the Materia Medica section at Hpathy.
None of these medicines should be taken without professional advice and guidance.
Homeopathy Remedies for Cholecystitis :
Card-m., chel., chion., chol., lach., lept., morg-g., myric., phos., podo., pyrog.
References
- ^ Derici H, Kara C, Bozdag AD, Nazli O, Tansug T, Akca E (2006). “Diagnosis and treatment of gallbladder perforation”. World J. Gastroenterol. 12 (48): 7832–6. PMID 17203529.
- Shea JA, Berlin JA, Escarce JJ, et al (November 1994). “Revised estimates of diagnostic test sensitivity and specificity in suspected biliary tract disease”. Arch. Intern. Med. 154 (22): 2573–81. PMID 7979854.
- Fink-Bennett D, Freitas JE, Ripley SD, Bree RL (August 1985). “The sensitivity of hepatobiliary imaging and real-time ultrasonography in the detection of acute cholecystitis”. Arch Surg 120 (8): 904–6. PMID 3893388.