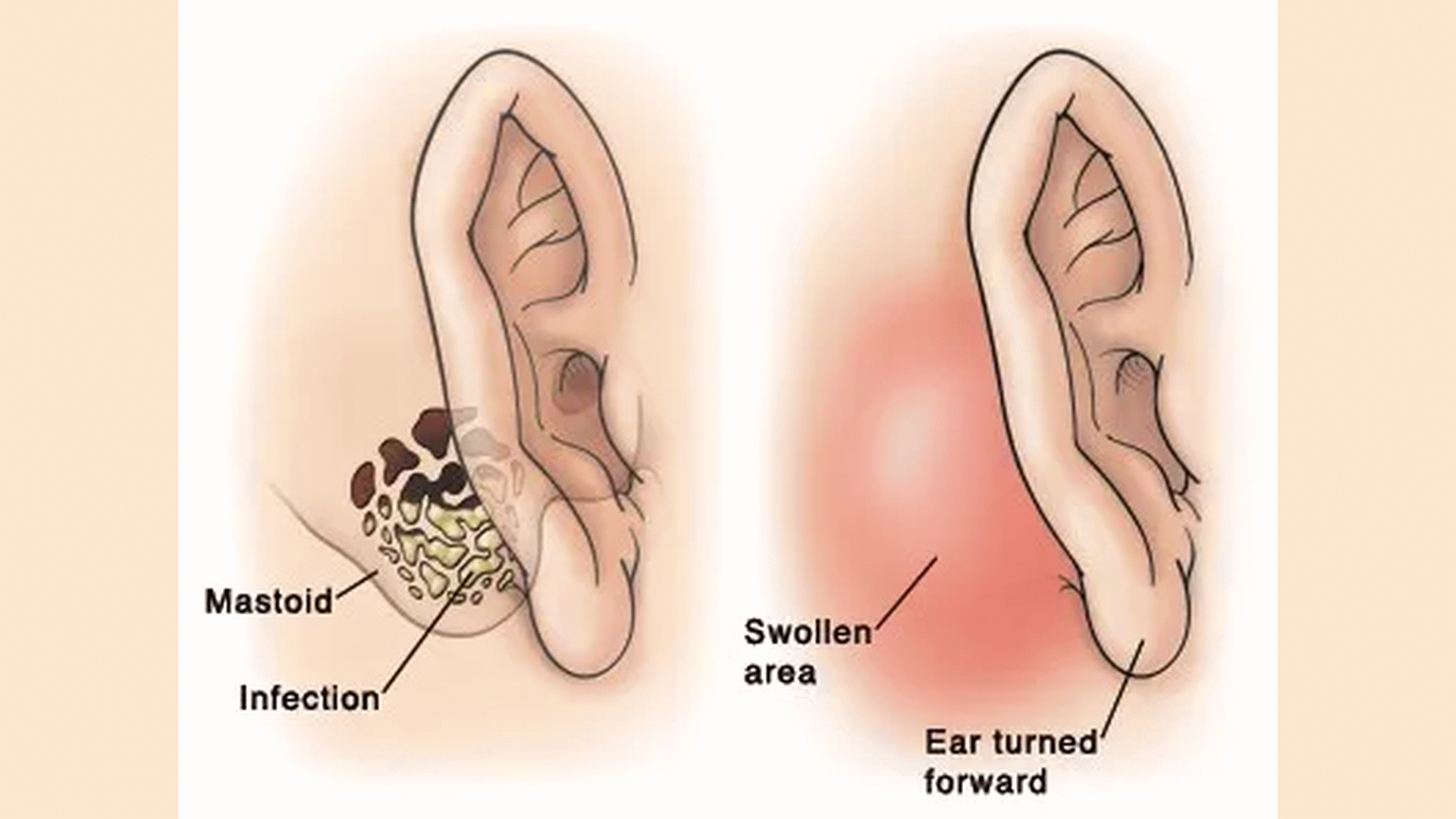
Mastoiditis is a serious bacterial infection and a complication of ear infection that affects the membrane lining of the mastoid bone in the skull, which is found behind the ear. This infection should be diagnosed and treated quickly with medications. Mastoiditis is more common in children. Most people with mastoiditis recover soon and have no complications as long as the mastoiditis is diagnosed and treated quickly.
There are two main types of mastoiditis: acute mastoiditis, which is the most common type and usually develops as a complication of a middle ear infection, and chronic mastoiditis, which is a long-term infection of the mastoid bone that often results from untreated acute mastoiditis.
The main symptom of mastoiditis is pain at the back of the ear, sometimes accompanied by swelling and fever. Mastoiditis should be treated with antibiotics to prevent the infection from spreading to the bone. If the bacteria spread, they can cause meningitis, an infection of the layers of the brain. This complication is life-threatening and must be treated immediately.
Role of homeopathy in mastoiditis
Homeopathy is often considered a complementary approach to managing mastoiditis. Individuals with mastoiditis should consult their homeopathic physician and explain their symptoms in detail. Always inform your doctor about complementary therapies you’re considering to ensure a well-rounded and safe approach to managing mastoiditis.
Seven effective homeopathic medicines for mastoiditis
Belladonna
Common name: Deadly nightshade
Belladonna is indicated in mastoiditis cases with acute inflammation, characterized by throbbing pain, heat, and redness around the affected area. Patients may experience sensitivity to touch, fever, and worsening pain with movement. This medicine is suitable for individuals who are restless and may have dilated pupils.
Hepar sulphuris calcareum
Common name: Calcium sulphide
Hepar sulph. is beneficial when there is pus formation in mastoiditis, along with extreme sensitivity to touch. Patients requiring this medicine often experience sharp, splinter-like pain and may feel like a splinter is stuck in the ear. Cold air increases the pain, and the affected ear may feel swollen and inflamed.
Silicea
Common name: Silica
Silicea is indicated in cases of chronic suppuration of mastoiditis with offensive discharge. It helps in expelling pus and promoting the healing process. Patients may experience slow healing, and the discharge may have a bad odor.
Pulsatilla
Common name: Windflower
Pulsatilla is suitable for cases with thick, yellow-green discharge and a diminished sense of smell and taste. Patients may crave fresh air and have no thirst. Symptoms of mastoiditis are often variable and may change frequently.
Mercurius solubilis
Common name: Quicksilver
Mercurius solubilis is useful in cases of mastoiditis with intense throbbing pain, offensive discharge, and excessive sweating. Pain worsens at night and with temperature changes. Patients may also experience a metallic taste in the mouth.
Calcarea sulphurica
Common name: Plaster of Paris / Sulphate of lime
Calcarea sulphurica is helpful in the later stages of mastoiditis when there is slow healing and thick, yellow pus discharge. It aids in the resolution of pus and promotes the healing process.
Arsenicum album
Common name: Arsenic trioxide
Arsenicum album is indicated when there is burning pain and restlessness, along with weakness and anxiety. It is useful in cases of mastoiditis with offensive discharge and chilly sensations. Patients may have a fear of death and may be meticulous and anxious about their condition of mastoiditis.
Causative factors of mastoiditis
Middle ear infection
Untreated or poorly treated middle ear infections can result in bacterial infections such as mastoiditis. Mastoiditis often occurs when bacteria from the middle ear infection spread to the mastoid bone behind the ear.
Bacteria
Common bacteria that cause middle ear infections include Streptococcus pneumoniae, Haemophilus influenzae, and Moraxella catarrhalis. If the infection caused by these bacteria is not treated properly, it can progress to mastoiditis. Individuals can catch these infections due to poor hygiene or average living standards.
Weak immune system
People with a weak immune system are prone to infections, including those in the middle ear, which can lead to mastoiditis. Individuals who have diseases such as HIV or AIDS are more vulnerable to such infections.
Repeated ear infections
People who experience frequent or recurrent ear infections are also at a higher risk of developing mastoiditis.
A foreign body or any obstruction
Problems with the middle ear’s drainage, such as anatomical issues or obstructions, can contribute to the development of mastoiditis. If the ear cannot properly drain fluid, bacteria may accumulate and cause an infection.
Symptoms of mastoiditis
Ear pain
Continuous pain in or behind the ear often worsens at night and upon chewing.
Redness and warmth
The skin around the affected ear might look red and feel warm on touch.
Fever
A high body temperature above 101 degrees Fahrenheit, usually with chills or sweating, indicates an infection.
Drainage of pus
Pus or fluid might come out of the ear canal, sometimes with a bad smell.
Hearing loss
Reduced ability to hear in the affected ear, which could be temporary or permanent depending on the severity or stage of mastoiditis.
Irritability
Mastoiditis can make children irritable or fussy because of pain and discomfort.
Swelling at the back of the ear
There is visible swelling or tenderness in the mastoid bone area, the bony part behind the ear.
Headache
Continuous headaches especially around the affected ear can occur due to mastoiditis.
Nausea and vomiting
Mastoiditis can lead to feeling sick and vomiting, especially if the infection spreads or causes more pressure on the skull.
Treatment of mastoiditis
Mastoiditis is managed using antibiotics and steroids. However, if antibiotics prove ineffective or there is an abscess or pus built up in the mastoid, surgery may be advised to eliminate the infected bone. Surgical options for mastoiditis may involve tympanostomy, where the surgeon inserts small hollow cylinders, known as ear tubes, into the eardrum. This procedure is effective in treating chronic middle ear infections and acute mastoiditis. Another surgical procedure is mastoidectomy, where the infected portion of the mastoid bone is removed or scraped out.
Diet and lifestyle modifications in mastoiditis
Consume anti-inflammatory foods
To reduce inflammation of mastoiditis and support the immune system, consume food rich in omega-3 fatty acids, like fish, flaxseeds, and walnuts, and antioxidants, like fruits and vegetables.
Avoid allergens
If allergies exacerbate mastoiditis symptoms, consider avoiding common allergens such as dairy, gluten, and certain foods that trigger allergic reactions.
Limit sugar and processed foods
These foods may lower the immune system and promote inflammation, potentially worsening mastoiditis symptoms.
Manage stress
Practice techniques such as meditation, deep breathing exercises, or yoga to help support overall immune function and reduce inflammation caused due to mastoiditis.
Avoid smoking
Smoking and secondhand smoke can increase respiratory symptoms and weaken the immunity, making it difficult for the body to fight infection of mastoiditis.
Maintain good hygiene
Wash your hands often, especially before touching your face or ears, to reduce the risk of spreading bacteria that could lead to ear infections.
Avoid putting foreign objects
A foreign object like a cotton bud, pencil, or safety pin may cause more problems to the ear and may develop further infection if it is already infected.
Conclusion
Mastoiditis is a grave consequence of untreated or improperly treated middle ear infection. It is identified by symptoms like ear pain, swelling at the back of the ear, fever, and hearing impairment. Seeking immediate medical attention is important to avoid potential complications of mastoiditis such as hearing loss, meningitis, or the formation of abscesses. While homeopathy can provide supportive care in symptom management and enhance overall well-being, it should always be utilized alongside a proper lifestyle modification and supervised by a qualified healthcare professional.
References
- Sahi D, Nguyen H, Callender KD. Mastoiditis. StatPearls Publishing; 2023. https://www.ncbi.nlm.nih.gov/books/NBK560877/
- Tyagi, Minali & Kumar, Dr. (2024). ROLE OF HOMOEOPATHY IN THE MANAGEMENT OF OTITIS MEDIA www.ijrar.org (EISSN 23481269, PISSN 23495138) IJRAR24A1146. 11. 8285. https://www.researchgate.net/publication/378003644_ROLE_OF_HOMOEOPATHY_IN_THE_MANAGEMENT_OF_OTITIS_MEDIA_wwwijrarorg_EISSN_23481269_PISSN_23495138_IJRAR24A1146
- Bhalerao, Rupali. (2011). Homeopathy for Ear infection. Vital Informer. 19. 2. https://www.researchgate.net/publication/221901665_Homoeopathy_for_Ear_nfection
- Mamatha C, Thangavel M. Otitis media – A review through its continuum through years and various treatment options [Internet]. Globalresearchonline.net. [cited 2024 Feb 23]. Available from: https://globalresearchonline.net/journalcontents/v45-1/46.pdf
- Bell IR, Boyer NN. Homeopathic medications as clinical alternatives for symptomatic care of acute otitis media and upper respiratory infections in children. Glob Adv Health Med [Internet]. 2013 [cited 2024 Feb 23];2(1):32–43. Available from: http://dx.doi.org/10.7453/gahmj.2013.2.1.007
- Gond DBP. Miasmatic approach in the treatment of chronic suppurative otitis media: A case report. Int J Homoeopathic Sci [Internet]. 2023;7(4):178–81. Available from: https://www.homoeopathicjournal.com/articles/973/7-4-26-908.pdf
- Sharma, Pawan & Aggarwal, Tanya & Kar, Shubhadeep. (2021). Study of 20 Cases of Otitis Media Successfully Treated with Homoeopathic Medicines—A Case Series. Homeopathic Links. 33. 309-317. 10.1055/s-0040-1718935.https://www.researchgate.net/publication/348154530_Study_of_20_Cases_of_Otitis_Media_Successfully_Treated_with_Homoeopathic_Medicines-A_Case_Series/citation/download
- Hasan, Nazmul & Ahsan, Nazmul & Sumit, Ahmed & Bari, Latiful & Akhand, Anwarul. (2021). Remedial Effects of Homeopathic Medicine in Chronic Suppurative Otitis Media-Related Complications. Bioresearch Communications. 7. 982-989. 10.3329/brc.v7i2.54372. https://www.researchgate.net/publication/352855889_Remedial_Effects_of_Homeopathic_Medicine_in_Chronic_Suppurative_Otitis_Media-Related_Complications/citation/download