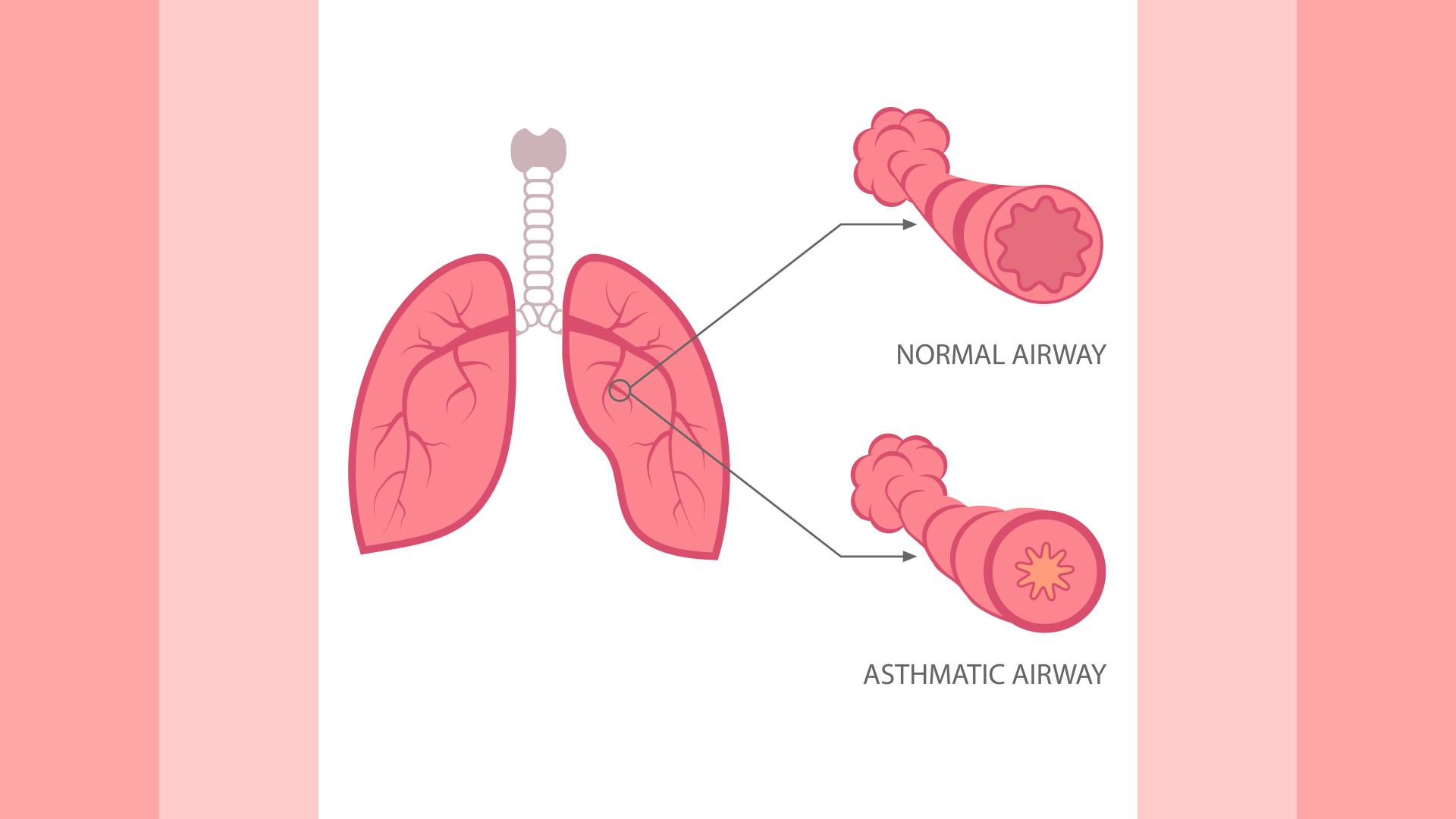
Bronchitis is an inflammatory condition of the airway tubes that carries air into your lungs from your trachea. The inflamed airway tubes make it difficult for the oxygen to get into your lungs, resulting in breathlessness. It often gets triggered by exposure to allergens.
Allergic bronchitis that lasts for more than three months is called chronic bronchitis. Acute or chronic bronchitis develops due to exposure to allergens such as dust, air pollutants, molds, tobacco smoke, and chemical fumes. However, acute bronchitis goes away within a few days to weeks.
Homeopathy is an effective mode of treatment for allergic bronchitis. It reduces inflammation in your bronchial tube and eases mucus expectoration. As your mucus is thrown out effortlessly, the chest pain, cough, and difficulty in breathing also subside.
These natural remedies provide you with long-lasting relief from allergic bronchitis
and prevent complications.
Role of homeopathy in allergic bronchitis
Homeopathic doctors treat allergic bronchitis using a constitutional approach based on symptoms and individualization. Constitutional homeopathic medicines for allergic bronchitis aim to correct the root cause and reduce the hypersensitivity of your immune system. Taking homeopathy for allergic bronchitis relieves your symptoms by decreasing inflammation in your airways and bronchial tubes.
Thus, homeopathic medications treat allergic bronchitis by preventing allergy and controlling episodes of allergic bronchitis. However, you should consult a homeopathic doctor first, who can evaluate your condition and prescribe suitable medications.
Top five homeopathic medicines for allergic bronchitis
Antimonium tartaricum (Ant-t.)
Common name: Tartar emetic
Ant. tart. is used to treat allergic bronchitis with a rattling cough. This homeopathic remedy is prescribed for the accumulation of excess mucus in the bronchial tubes. The characteristic symptom of Ant. tart. is white and frothy phlegm that is expectorated with great difficulty. Often, the expectoration has a sour or salty taste.
Ant. tart. works well in people with chest pain, suffocation, and constriction due to allergic bronchitis. This remedy is indicated when the cough is relieved after expectoration, burping, spitting, lying on the right side, or sitting up.
Arsenic album (Ars. alb.)
Common name: Arsenious acid
Ars. alb. is used for allergic bronchitis with marked wheezing in the chest and cough. There is a tight feeling of constriction in the chest with marked anxiety and restlessness.
Allergic bronchitis with a burning sensation in the chest can be relieved by Ars. alb. Cough that worsens at night and upon lying down, making respiration difficult, is the keynote symptom of this remedy. It compels the person to sit up at night. Expectoration is often scanty, white, tenacious mucus or mucus lumps. Ars. alb. expectoration is bitter or salty to taste.
Hepar sulphuris calcareum
Common name: Hahnemann’s calcium sulfide
Hepar sulph. is recommended for allergic bronchitis with loose, deep, violent, rattling cough with wheezing. Copious expectoration of tenacious mucus brings relief to rattling cough. Wrapping up the body with warm clothes gives relief.
There is a feeling of tightness in the chest that leads to upper body pains. Cough gets worse in the cold air or from taking cold drinks. Hepar sulph. expectoration often has a fetid smell and a sour/sweet taste.
Pulsatilla nigricans (Puls.)
Common name: Windflower
Allergic bronchitis with a feeling of weight in the chest is indicative of Pulsatilla. Cough with thick yellow mucus and a sensation of choking and gagging responds well to this remedy. It is often dry or tight at night and becomes loose in the morning.
Cough worsens in a stuffy room and is relieved in the open air. Pulsatilla is often helpful in allergic bronchitis with fever in the evening towards night with low thirst.
Natrium muriaticum (Nat-m.)
Common name: Chloride of sodium
Nat. mur. is indicated for allergic bronchitis with white expectoration, especially in the morning. The cough is short, and phlegm is coughed up with difficulty. There is wheezing and breathing difficulty with transparent mucus.
Nat. mur. yields good results in allergic bronchitis with the sensation of oppression in the chest or sore, bruised pain in the chest. These people experience stitches in the chest upon deep inspiration. Nat. mur. expectoration has a salty taste.
Causes for allergic bronchitis
Allergens
- Pollen from trees, grasses, and weeds can trigger allergic bronchitis.
- Dust mites (tiny organisms that thrive in dust) found in bedding, upholstered furniture, and carpets can initiate allergic bronchitis.
- Mold spores found both indoors and outdoors, particularly in your bathrooms, basements, and other areas with high humidity can be the cause for allergic bronchitis.
- Pet dander, such as proteins found in pets’ skin flakes, urine, feces, and saliva (dogs, cats, rodents, and birds), can also trigger allergic bronchitis.
- Cockroach droppings or particles from cockroach waste can be airborne and act as allergens.
Airborne irritants
- If you are a smoker or are exposed to passive tobacco smoke, it can irritate your bronchial tubes, causing allergic bronchitis.
- Exposure to pollutants like vehicle exhaust, industrial emissions, and other airborne chemicals can worsen your allergic bronchitis.
Respiratory infections
While not directly causing allergic bronchitis, infections such as colds, flu, or sinusitis can worsen bronchial inflammation.
Weather changes
Changes in weather conditions, like cold air, can trigger your bronchial inflammation and worsen your symptoms.
Food allergies
If you have food allergies, it can lead to respiratory symptoms, including allergic bronchitis.
Genetic predisposition
If you have a family history of allergies or asthma, you may be more susceptible to allergic bronchitis.
Symptoms of allergic bronchitis
Coughing
A persistent cough is a hallmark symptom, often dry initially, but as allergic bronchitis progresses, it gets clear, white, or yellow mucus.
Wheezing
The narrowing of your airways along with inflammation causes wheezing.
Shortness of breath
You may experience breathlessness due to inflammation and narrowing of the airways.
Excess mucus production
In allergic bronchitis, you may produce more mucus than usual. It can be clear, white, yellow, or greenish.
Sore throat
Due to postnasal drip in allergic bronchitis, you may have a sore or itchy throat.
Nasal congestion
You might also experience a runny nose or sneezing when triggered by airborne allergens. This allergic reaction can also affect your eyes, which might itch or get red or watery.
Treatment for allergic bronchitis
The treatment for allergic bronchitis mainly aims to open up your airways and help you breathe easily.
Bronchodilators
Bronchodilators relax muscles around your airways to open them. You breathe these medications through an inhaler. There are two kinds of bronchodilators.
- Short-acting bronchodilators act quickly.
- Long-acting bronchodilators that take time to act, but their impact lasts longer.
Steroids
Steroids reduce swelling in your airways. These are administered through an inhaler. Steroids, along with long-acting bronchodilators, can be prescribed to you for better relief in allergic bronchitis.
Oxygen therapy
This delivers oxygen to your lungs to assist you in breathing. Depending on your oxygen saturation, your doctor will decide if you need oxygen therapy.
Humidifier
Warm mist humidifiers help you breathe, especially at night, by loosening up the mucus in your airways.
Vaccines
The risk of lung infections increases if you have allergic bronchitis. Discuss with your physician about getting a flu shot, and pneumonia shot to help you stay healthy.
Diet and lifestyle modifications for allergic bronchitis
Avoid Allergens
The most important lifestyle change for allergic bronchitis is identifying and avoiding allergens that trigger your symptoms.
- Check for all common allergens like pollen, dust mites, pet dander, mold, and certain foods.
- Regularly clean your living space, and use air purifiers.
- Consider using allergen-proof covering for your pillows and mattresses.
Pulmonary rehabilitation
This programme includes:
- Exercises improve your breathing, improve lung function, reduce breathlessness, and enhance oxygen exchange.
- Healthy nutrition including foods rich in anti-inflammatory properties help to reduce inflammation in your bronchial tubes.
- Drinking sufficient water to ease thin mucus secretions and make it easy to expel.
Breathing techniques
Allergic bronchitis changes your breathing pattern to quick breathing. Practicing breathing techniques like pursed-lip breathing can help you slow your breathing rate. Also, you can try diaphragmatic breathing. It improves lung function, reduces shortness of breath, and enhances oxygen exchange.
Conclusion
Immune response and inflammation are defense mechanisms that protect us. However, when this becomes excessive, it can be distressing and sometimes fatal.
One of the effective modes of treating allergic bronchitis is homeopathy. Try homeopathy to prevent allergic bronchitis episodes.
References
- Singh A, Avula A, Zahn E. Acute Bronchitis. StatPearls Publishing; 2023. https://www.ncbi.nlm.nih.gov/books/NBK448067/
- Colin P. Homeopathy and respiratory allergies: a series of 147 cases. Homeopathy [Internet]. 2006;95(2):68–72. Available from: https://www.sciencedirect.com/science/article/pii/S1475491606000129
- Bellavite, P., Ortolani, R., Pontarollo, F., Piasere, V., Benato, G., & Conforti, A. (2006). Immunology and homeopathy. 4. Clinical studies—part 2. Evidence-Based Complementary and Alternative Medicine: eCAM, 3(4), 397–409. https://doi.org/10.1093/ecam/nel046
- Homeopathy [Internet]. NCCIH. [cited 2024 Jan 3]. Available from: https://www.nccih.nih.gov/health/homeopathy
- Ullman, Dana & Frass, Michael. (2010). A Review of Homeopathic Research in the Treatment of Respiratory Allergies. Alternative medicine review : a journal of clinical therapeutic. 15. 48-58. Available from:https://www.researchgate.net/publication/42832498_A_Review_of_Homeopathic_Research_in_the_Treatment_of_Respiratory_Allergies/citation/download
- Enos C. Nih.gov. [cited 2024 Jan 3]. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9725525/pdf/homoeopathphys132126-0026.pdf
- Zanasi A, Mazzolini M, Tursi F, Morselli-Labate AM, Paccapelo A, Lecchi M. Homeopathic medicine for acute cough in upper respiratory tract infections and acute bronchitis: A randomized, double-blind, placebo-controlled trial. Pulm Pharmacol Ther [Internet]. 2014 [cited 2024 Jan 3];27(1):102–8. Available from: https://pubmed.ncbi.nlm.nih.gov/23714686/
- Varanasi, Roja & Gupta, Jaya & M, Prakash & K, Raju & Prasad, R & Sadanandan, Gopinadhan & Arya, J & Mandal, B & Singh, Mohan & Singh, Vikram & Nayak, Chaturbhuja & Pramanik, Abhishek & Kumar, Arvind. (2021). Management of early years of simple and mucopurulent chronic bronchitis with pre-defined Homoeopathic medicines – a Prospective Observational Study with 2-Years Follow-Up: homeopathy for management of chronic bronchitis. International Journal of High Dilution Research – ISSN 1982-6206. 18. 47-62. 10.51910/ijhdr.v18i3-4.973. https://www.researchgate.net/publication/350593410_Management_of_early_years_of_simple_and_mucopurulent_chronic_bronchitis_with_pre-defined_Homoeopathic_medicines_-_a_Prospective_Observational_Study_with_2-Years_Follow-Up_homeopathy_for_management_of_/citation/download
- Singh A, Avula A, Zahn E. Acute Bronchitis. StatPearls Publishing; 2023.https://www.ncbi.nlm.nih.gov/books/NBK448067/
- Lopuhaä CE, Out TA, Jansen HM, Aalberse RC, Van Der Zee JS. Allergen?induced bronchial inflammation in house dust mite?allergic patients with or without asthma. Clin Exp Allergy [Internet]. 2002 [cited 2024 Jan 3];32(12):1720–7. Available from: https://pubmed.ncbi.nlm.nih.gov/12653162
- Fisk WJ, Eliseeva EA, Mendell MJ. Association of residential dampness and mold with respiratory tract infections and bronchitis: a meta-analysis. Environ Health [Internet]. 2010 [cited 2024 Jan 3];9(1):72. Available from: http://dx.doi.org/10.1186/1476-069x-9-72
- Brunekreef B, Groot B, Hoek G. Pets, allergy and respiratory symptoms in children. Int J Epidemiol [Internet]. 1992 [cited 2024 Jan 3];21(2):338–42. Available from:https://pubmed.ncbi.nlm.nih.gov/1428490/
- Strzelak A, Ratajczak A, Adamiec A, Feleszko W. Tobacco smoke induces and alters immune responses in the lung triggering inflammation, allergy, asthma, and other lung diseases: A mechanistic review. Int J Environ Res Public Health [Internet]. 2018 [cited 2024 Jan 3];15(5):1033. Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5982072/
- Takizawa H. Impact of air pollution on allergic diseases. Korean J Intern Med [Internet]. 2011 [cited 2024 Jan 3];26(3):262. Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3192198/
- Hyrkäs-Palmu H, Ikäheimo TM, Laatikainen T, Jousilahti P, Jaakkola MS, Jaakkola JJK. Cold weather increases respiratory symptoms and functional disability especially among patients with asthma and allergic rhinitis. Sci Rep [Internet]. 2018 [cited 2024 Jan 3];8(1). Available from: http://dx.doi.org/10.1038/s41598-018-28466-y
- Ober C, Yao T-C. The genetics of asthma and allergic disease: a 21st century perspective. Immunol Rev [Internet]. 2011 [cited 2024 Jan 3];242(1):10–30. Available from: http://dx.doi.org/10.1111/j.1600-065x.2011.01029.x
- Almadhoun K, Sharma S. Bronchodilators. StatPearls Publishing; 2023.https://www.ncbi.nlm.nih.gov/books/NBK519028/
- Hawkins DB, Crockett DM, Shum TK. Corticosteroids in airway management. Otolaryngol Head Neck Surg [Internet]. 1983 [cited 2024 Jan 3];91(6):593–6. Available from:https://pubmed.ncbi.nlm.nih.gov/6198612/
- Liu K, Li S, Qian Z (min), Dharmage SC, Bloom MS, Heinrich J, et al. Benefits of influenza vaccination on the associations between ambient air pollution and allergic respiratory diseases in children and adolescents: New insights from the Seven Northeastern Cities study in China. Environ Pollut [Internet]. 2020;256(113434):113434. Available from: https://www.sciencedirect.com/science/article/abs/pii/S0269749119328301#:~:text=Conclusions,of%20reduced%20allergic%20respiratory%20diseases.
- Tereziu S, Minter DA. Pneumococcal Vaccine. StatPearls Publishing; 2023.https://www.ncbi.nlm.nih.gov/books/NBK507794/
- Pulmonary rehabilitation [Internet]. NHLBI, NIH. [cited 2024 Jan 3]. Available from: https://www.nhlbi.nih.gov/health/pulmonary-rehabilitation).
- Nguyen JD, Duong H. Pursed-lip breathing. StatPearls Publishing; 2023.https://www.ncbi.nlm.nih.gov/books/NBK545289/
- Hamasaki H. Effects of diaphragmatic breathing on health: A narrative review. Medicines (Basel) [Internet]. 2020 [cited 2024 Jan 3];7(10):65. Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7602530/